Hammer Toe Operation Complications
 Overview
Overview
A hammer toe can be defined as a condition that causes your toe to bend downward instead of pointing forward. While it can occur on any toe on your foot, it usually affects the second or third toe. If your baby toe curls instead of buckling, it is also considered a hammer toe. There are two types of hammer toes. If your toes still can move around at the joint, then it is considered a flexible hammer toe. It is a milder form of the condition and there are more treatment options. The other type is called a rigid hammertoes, which occurs when the tendons in your toe become so rigid that they push your toe joint out of alignment, and it cannot move at all. Typically, you will need surgery to fix it.
Causes
Medical problems, such as stroke or diabetes that affect the nerves, may also lead to hammertoe. For example, diabetes can result in poor circulation, especially in the feet. As a result, the person may not feel that their toes are bent into unnatural positions. The likelihood of developing hammertoe increases with age and may be affected by gender (more common in women) and toe length; for example, when the second toe is longer than the big toe, hammertoe is more likely to occur. Hammertoe may also be present at birth. Genetics may factor in to developing hammertoe, particularly if the foot is flat or has a high arch, resulting in instability.
 Symptoms
Symptoms
Symptoms include sharp pain in the middle of the toe and difficulty straightening the toe. People with hammertoe may also develop blisters, which are fluid-filled pockets of skin, because the bent toe is likely to rub against the inside of a shoe. This increased friction may also lead to calluses, which are areas of thickened skin, and corns, which are hard lumps that may form on or between toes. Symptoms may be minor at first, but they can worsen over time.
Diagnosis
Hammertoes are progressive, they don?t go away by themselves and usually they will get worse over time. However, not all cases are alike, some hammertoes progress more rapidly than others. Once your foot and ankle surgeon has evaluated your hammertoes, a treatment plan can be developed that is suited to your needs.
Non Surgical Treatment
Any forefoot problems that cause pain or discomfort should be given prompt attention. Ignoring the symptoms can aggravate the condition and lead to a breakdown of tissue, or possibly even infection. Conservative treatment of mallet toes begins with accommodating the deformity. The goal is to relieve pressure, reduce friction, and transfer forces from the sensitive areas. Shoes with a high and broad toe box (toe area) are recommended for people suffering from forefoot deformities such as mallet toes. This prevents further irritation in the toe area from developing. Other conservative treatment includes forefoot supports such as gel toe caps, gel toe shields and toe crests. Gel forefoot supports provide immediate comfort and relief from common forefoot disorders without drying the skin.
Surgical Treatment
Hammertoe surgery is performed when conservative measures have been exhausted and pain or deformity still persists. The surgery is performed on an outpatient basis. It typically required about one hour of time. An incision is placed over the inter-phalangeal joint. Once the bone is exposed, the end portion of the bone is removed. Your surgeon may then use pins or other fixation devices to assist in straightening the toe. These Hammer toe devices may be removed at a later date if necessary. Recovery for hammertoe surgery is approximately 10 to 14 days. You are able to walk immediately following the surgery in a surgical shoe. Swelling may be present but is managed as needed. Physical therapy is used to help reduce swelling in the toe or toes after surgery. Most of these toe surgeries can be performed in the office or the outpatient surgery under local anesthesia.
 Prevention
Prevention
Skin creams can help maintain skin softness and pliability. A pumice stone or loofah sponge can help get rid of dead skin. Taking a warm footbath for 10 minutes two or three times a week will keep the feet relaxed and help prevent mild foot pain caused by fatigue. Adding 1/2 cup of Epsom salts increases circulation and adds other benefits. Taking footbaths only when the feet are painful is not as helpful.
Over-Pronation
Overview
Pronation is the natural act of the body spreading the impact of walking, jogging or running throughout the foot evenly. As the foot strikes the ground, the ankle naturally rolls inward absorbing the shock of the ground and mobilizing to the terrain. Overpronation is when the ankle of the foot rolls in past its normal 15? of inward rotation. The cause of this could be many things such as foot type, biomechanics, or compensation strategies. People with flat feet often, although not always, overpronate.
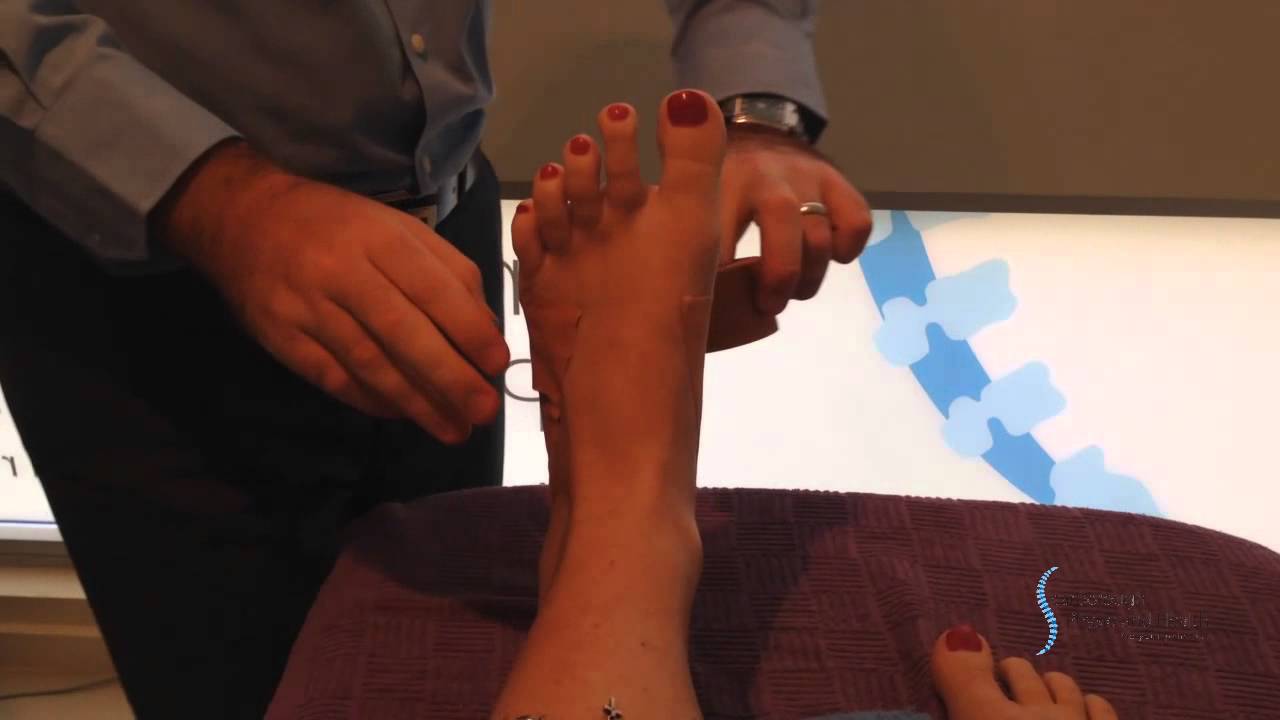
Causes
There are many possible causes for overpronation, but researchers have not yet determined one underlying cause. Hintermann states, Compensatory overpronation may occur for anatomical reasons, such as a tibia vara of 10 degrees or more, forefoot varus, leg length discrepancy, ligamentous laxity, or because of muscular weakness or tightness in the gastrocnemius and soleus muscles. Pronation can be influenced by sources outside of the body as well. Shoes have been shown to significantly influence pronation. Hintermann states that the same person can have different amounts of pronation just by using different running shoes. It is easily possible that the maximal ankle joint eversion movement is 31 degrees for one and 12 degrees for another running shoe.
Symptoms
Because pronation is a twisting of the foot, all of the muscles and tendons which run from the leg and ankle into the foot will be twisted. In over-pronation, resulting laxity of the soft tissue structures of the foot and loosened joints cause the bones of the feet shift. When this occurs, the muscles which attach to these bones must also shift, or twist, in order to attach to these bones. The strongest and most important muscles that attach to our foot bones come from our lower leg. So, as these muscles course down the leg and across the ankle, they must twist to maintain their proper attachments in the foot. Injuries due to poor biomechanics and twisting of these muscles due to over-pronation include: shin splints, Achilles Tendonitis, generalized tendonitis, fatigue, muscle aches and pains, cramps, ankle sprains, and loss of muscular efficiency (reducing walking and running speed and endurance). Foot problems due to over-pronation include: bunions, heel spurs, plantar fasciitis, fallen and painful arches, hammer toes, and calluses.
Diagnosis
The best way to discover whether you have a normal gait, or if you overpronate, is to visit a specialty run shop, an exercise physiologist, a podiatrist or a physical therapist who specializes in working with athletes. A professional can analyze your gait, by watching you either walk or run, preferably on a treadmill. Some facilities can videotape your gait, then analyze the movement of your feet in slow-motion. Another (and less costly) way is to look at the bottom of an older pair of run shoes. Check the wear pattern. A person with a normal gait will generally see wear evenly across the heel and front of the shoe. A person who overpronates will likely see more wear on the OUTside of the heel and more wear on the INside of the forefoot (at the ball). A person who supinates will see wear all along the outer edges of the shoe. You can also learn about your gait by looking at your arches. Look at the shape your wet feet leave on a piece of paper or a flat walking surface.

Non Surgical Treatment
Get a gait analysis of your running style, this will highlight if you overpronate, oversupinate or have a neutral gait. Most podiatrists, physio's and sports therapists will offer this service, as do some specialist sports shops. Find a clinic. If you overpronate, get orthotics with extra medial support. Many running shoes have a harder material on the inside of the midsole (the thick hard foam part of the running shoe). This means the inside of the shoe will be compressed less under load and support the inside of the foot preventing it from rolling in or flattening. For people with considerable overpronation, another option is to have an orthotic device fitted. Orthotic insoles come in many types and prices. Some are pre-molded and can be bought off the shelf. These are ok for the majority of problem feet. However some cases may require specially casted orthotics from a relevant sports injury therapist or podiatrist.
Prevention
Pronation forces us to bear most of our weight on the inner border of our feet. Custom-made orthotics gently redistributes the weight so that the entire foot bears its normal share of weight with each step we take. The foot will not twist out at the ankle, but will strike the ground normally when the orthotics is used. This action of the custom-made orthotics will help to prevent shin splints, ankle sprains, knee and hip pain, lower back pain, nerve entrapments, tendonitis, muscle aches, bunions, generalized fatigue, hammer toes, and calluses.
Dealing With Severs Disease
Overview
Sever?s disease is a painful condition of the heel affecting children, usually at the beginning of the growth spurt in early puberty. It is caused by inflammation at the growth plate at the back of the heel, adjacent to the Achilles tendon attachment. This is one of the most common causes of heel pain in school-aged children. Physically active children aged between eight and fourteen years old are most at risk of developing pain from Sever?s disease. It is common among children involved in soccer, little athletics, gymnastics, basketball and netball but can affect children involved in any running or jumping activity. Boys seem to be more commonly affected than girls.
Causes
Apart from age, other factors that may contribute to developing Sever?s disease include physical activity, any form of exercise that is weight bearing through the legs or stresses the soft tissue can exacerbate the pain of the disease, External factors, for example, running on hard surfaces or wearing inappropriate shoes during sport Overuse injury, very active children may repeatedly but subtly injure the bones, muscles and tendons of their feet and ankles. In time, the accumulated injuries cause symptoms.
Symptoms
A few signs and symptoms point to Sever?s disease, which may affect one or both heels. These include pain at the heel or around the Achilles tendon, Heel pain during physical exercise, especially activities that require running or jumping, worsening of pain after exercise, a tender swelling or bulge on the heel that is sore to touch, calf muscle stiffness first thing in the morning, limping, a tendency to tiptoe.
Diagnosis
Sever?s disease can be diagnosed based on the symptoms your child has. Your child?s doctor will conduct a physical examination by squeezing different parts of your child?s foot to see if they cause any pain. An X-ray may be used to rule out other problems, such as a broken bone or fracture.
Non Surgical Treatment
Sever?s disease will go away on its own with rest or after heel bone growth is complete, usually within 2 to 8 weeks after the heel pain or discomfort appears. Sever?s disease is not expected to cause long-term problems, though symptoms may linger for up to several years in severe cases. Certain conservative care measures may be helpful in treating this health problem, including avoiding activities that provoke pain or discomfort, elevating the leg while at rest, performing hamstring and calf muscle stretches two to three times per day, undergoing physical therapy, using cold therapy, using an elastic wrap or compression stocking, Avoiding footwear with heel elevation, toe spring, and toe taper, and instead favoring footwear that?s completely flat and widest at the ends of the toes. More aggressive treatment measures, including over-the-counter anti-inflammatory medication (e.g. ibuprofen), steroid injections, and surgery, may be indicated in certain cases. Addressing the footwear component of this health problem is an important part of a well-rounded Sever?s disease treatment plan. Optimal footwear for preventing or treating this problem is flat, wide (widest at the ends of the toes), and flexible in the sole. Open-back footwear (such as certain Crocs models) may be particularly helpful for kids and teens with Sever?s disease.
What Causes Heel Serious Pain
Overview

Your foot is made up of 26 bones, 33 joints, and more than 100 tendons. The heel is the largest bone in your foot. If you overuse or injure your heel, you may experience Heel Pain. This can range from mild to disabling. In many cases, if you have heel pain, you will need a doctor to diagnose the cause.
Causes
The most common cause of heel pain is plantar fasciitis. Plantar fasciitis is a stretching of the plantar fascia, a ligament that runs from the ball of foot through the arch and is attached to the heel. It is that attachment which becomes aggravated and typically causes pain after being on your feet for lengths of time. Abnormal motion of the foot (pronation) is one cause of plantar fasciitis. Heel spurs, which are abnormal bone growths coming off the heel, can also cause heel pain. Other causes include repetitive stress or shock to the heel, standing for prolonged periods or osteoarthritis.
Symptoms
Common symptoms, heel Spurs: the pain is usually worst on standing, particularly first thing in the morning when you get up. It is relatively common, though usually occurring in the over forty's age group. There are no visible features on the heel but a deep localised painful spot can be found in or around the middle of the sole of the heel. Although it is often associated with a spur of bone sticking out of the heel bone (heel spur syndrome), approximately ten per cent of the population have heel spurs without any pain. Heel Bursitis, pain can be felt at the back of the heel when the ankle joint is moved and there may be a swelling on both sides of the Achilles tendon. Or you may feel pain deep inside the heel when it makes contact with the ground. Heel Bumps, recognised as firm bumps on the back of the heel , they are often rubbed by shoes causing pain.
Diagnosis
Depending on the condition, the cause of heel pain is diagnosed using a number of tests, including medical history, physical examination, including examination of joints and muscles of the foot and leg, X-rays.
Non Surgical Treatment
Most heel pain is caused by a combination of poor biomechanics, or muscle weakness or tightness. The good news is that heel pain can be effectively managed once the cause is identified. Most heel pain can be successfully treated via pain and pressure relief techniques, biomechanical correction eg orthotics, taping, foot posture exercises, muscle stretches and massage, lower limb muscle strengthening, proprioceptive and balance exercises to stimulate your foot intrinsic muscles. If you feel that your footwear or sports training schedule are potentially causing your heel pain, then we recommend that you seek the advice of a sports physiotherapist, podiatrist or trained footwear specialist (not just a shop assistant) to see if your shoe is a match for your foot; or discuss your training regime to see if you are doing too much. Heel pain and injury are extremely common. With accurate assessment and early treatment most heel pain injuries respond extremely quickly to physiotherapy allowing you to quickly resume pain-free and normal activities of daily living. Please ask you physiotherapist for their professional treatment advice.
Surgical Treatment
If treatment hasn't worked and you still have painful symptoms after a year, your GP may refer you to either an orthopaedic surgeon, a surgeon who specialises in surgery that involves bones, muscles and joints or a podiatric surgeon, a podiatrist who specialises in foot surgery. Surgery is sometimes recommended for professional athletes and other sportspeople whose heel pain is adversely affecting their career. Plantar release surgery is the most widely used type of surgery for heel pain. The surgeon will cut the fascia to release it from your heel bone and reduce the tension in your plantar fascia. This should reduce any inflammation and relieve your painful symptoms. Surgery can be performed either as open surgery, where the section of the plantar fascia is released by making a cut into your heel or endoscopic or minimal incision surgery - where a smaller incision is made and special instruments are inserted through the incision to gain access to the plantar fascia. Endoscopic or minimal incision surgery has a quicker recovery time, so you will be able to walk normally much sooner (almost immediately), compared with two to three weeks for open surgery. A disadvantage of endoscopic surgery is that it requires both a specially trained surgical team and specialised equipment, so you may have to wait longer for treatment than if you were to choose open surgery. Endoscopic surgery also carries a higher risk of damaging nearby nerves, which could result in symptoms such as numbness, tingling or some loss of movement in your foot. As with all surgery, plantar release carries the risk of causing complications such as infection, nerve damage and a worsening of your symptoms after surgery (although this is rare). You should discuss the advantages and disadvantages of both techniques with your surgical team.
Prevention

It is not always possible to prevent heel pain, but there are measures you can take to help avoid further episodes. Being overweight can place excess pressure and strain on your feet, particularly on your heels. This increases the risk of damaging your feet and heels. If you are overweight, losing weight and maintaining a healthy weight by combining regular exercise with a healthy, balanced diet can be beneficial for your feet. You can calculate your body mass index (BMI) to find out whether you are a healthy weight for your height and build. To work out your BMI, divide your weight in kilograms by your height in metres squared. A BMI of less than 18.5 means that you are underweight, 18.5-24.9 means that your weight is healthy, 25-29 means that you are overweight, 30-40 means that you are obese, over 40 means that you are morbidly obese. You can also use the BMI healthy weight calculator to work out your BMI.
The Major Causes And Solutions For Achilles Tendinitis
Overview
 Achilles tendonitis is one of the most common running injuries. The achilles tendon is the large tendon at the back of the ankle. It connects the calf muscles made up of the gastrocnemius and soleus to the heel bone or calcaneus. It provides the power in the push off phase of walking and running where huge forces are transmitted through the achilles tendon. Achilles tendonitis is often now referred to as achilles tendinopathy. This is because the term tendinopathy covers all types of overuse achilles tendon injury. Strictly speaking tendonitis suggests an inflammatory condition of the tendon but in reality few achilles tendon injuries are actually down to pure inflammation. Soleus muscleThe main finding, particularly in older athletes is usually degeneration of the tissue with a loss of normal fibre structure. Other very similar conditions may actually be due to inflammation or degeneration of the tendon sheath which surrounds the tendon rather than the achilles tendon itself. In addition to being either chronic or acute, achilles tendonitis can also be at the attachment point to the heel called insertional achilles tendonitis or in the mid-portion of the tendon typically around 4cm above the heel. Healing of the achilles tendon is often slow, due to its poor blood supply.
Achilles tendonitis is one of the most common running injuries. The achilles tendon is the large tendon at the back of the ankle. It connects the calf muscles made up of the gastrocnemius and soleus to the heel bone or calcaneus. It provides the power in the push off phase of walking and running where huge forces are transmitted through the achilles tendon. Achilles tendonitis is often now referred to as achilles tendinopathy. This is because the term tendinopathy covers all types of overuse achilles tendon injury. Strictly speaking tendonitis suggests an inflammatory condition of the tendon but in reality few achilles tendon injuries are actually down to pure inflammation. Soleus muscleThe main finding, particularly in older athletes is usually degeneration of the tissue with a loss of normal fibre structure. Other very similar conditions may actually be due to inflammation or degeneration of the tendon sheath which surrounds the tendon rather than the achilles tendon itself. In addition to being either chronic or acute, achilles tendonitis can also be at the attachment point to the heel called insertional achilles tendonitis or in the mid-portion of the tendon typically around 4cm above the heel. Healing of the achilles tendon is often slow, due to its poor blood supply.
Causes
Achilles tendinitis may be caused by intensive hill running, sprinting, or stair climbing. Overuse resulting from the natural lack of flexibility in the calf muscles. Rapidly increasing intensity of exercise, especially after a period of inactivity. Sudden and hard contraction of the calf muscles when exerting extra effort, like that in a final sprint or high jump.
Symptoms
Patients with an Achilles tendon rupture frequently present with complaints of a sudden snap in the lower calf associated with acute, severe pain. The patient reports feeling like he or she has been shot, kicked, or cut in the back of the leg, which may result in an inability to ambulate further. A patient with Achilles tendon rupture will be unable to stand on his or her toes on the affected side. Tendinosis is often pain free. Typically, the only sign of the condition may be a palpable intratendinous nodule that accompanies the tendon as the ankle is placed through its range of motion (ROM). Patients with paratenonitis typically present with warmth, swelling, and diffuse tenderness localized 2-6 cm proximal to the tendon's insertion. Paratenonitis with tendinosis. This is diagnosed in patients with activity-related pain, as well as swelling of the tendon sheath and tendon nodularity.
Diagnosis
In diagnosing Achilles tendonitis or tendonosis, the surgeon will examine the patient?s foot and ankle and evaluate the range of motion and condition of the tendon. The extent of the condition can be further assessed with x-rays or other imaging modalities.
Nonsurgical Treatment
Tendinitis usually responds well to self-care measures. But if your signs and symptoms are severe or persistent, your doctor might suggest other treatment options. If over-the-counter pain medications - such as ibuprofen (Advil, Motrin IB, others) or naproxen (Aleve) - aren't enough, your doctor might prescribe stronger medications to reduce inflammation and relieve pain. A physical therapist might suggest some of the following treatment options. Exercises. Therapists often prescribe specific stretching and strengthening exercises to promote healing and strengthening of the Achilles tendon and its supporting structures. Orthotic devices. A shoe insert or wedge that slightly elevates your heel can relieve strain on the tendon and provide a cushion that lessens the amount of force exerted on your Achilles tendon.

Surgical Treatment
Surgical treatment for tendons that fail to respond to conservative treatment can involve several procedures, all of which are designed to irritate the tendon and initiate a chemically mediated healing response. These procedures range from more simple procedures such as percutaneous tenotomy61 to open procedures and removal of tendon pathology. Percutaneous tenotomy resulted in 75% of patients reporting good or excellent results after 18 months. Open surgery for Achilles tendinopathy has shown that the outcomes are better for those tendons without a focal lesion compared with those with a focal area of tendinopathy.62 At 7 months after surgery, 67% had returned to physical activity, 88% from the no-lesion group and 50% from the group with a focal lesion.
Prevention
You can take measures to reduce your risk of developing Achilles Tendinitis. This includes, Increasing your activity level gradually, choosing your shoes carefully, daily stretching and doing exercises to strengthen your calf muscles. As well, applying a small amount ZAX?s Original Heelspur Cream onto your Achilles tendon before and after exercise.
What Triggers Heel Pain And How To Prevent It
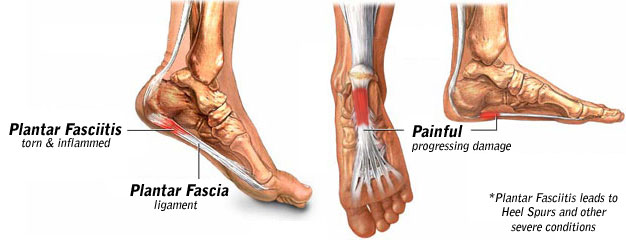
Overview
If your first few steps out of bed in the morning cause severe pain in the heel of your foot, you may have plantar fasciitis, an overuse injury that affects the sole of the foot. A diagnosis of plantar fasciitis means you have inflamed the tough, fibrous band of tissue (fascia) connecting your heel bone to the base of your toes.
Causes
Although plantar fasciitis may result from a variety of factors, such as repeat hill workouts and/or tight calves, many sports specialists claim the most common cause for plantar fasciitis is fallen arches. The theory is that excessive lowering of the arch in flat-footed runners increases tension in the plantar fascia and overloads the attachment of the plantar fascia on the heel bone (i.e., the calcaneus). Over time, the repeated pulling of the plantar fascia associated with excessive arch lowering is thought to lead to chronic pain and inflammation at the plantar fascia’s attachment to the heel. In fact, the increased tension on the heel was believed to be so great that it was thought to eventually result in the formation of a heel spur.
Symptoms
Plantar fascia usually causes pain and stiffness on the bottom of your heel although some people have heel spurs and suffer no symptoms at all. Occasionally, heel pain is also associated with other medical disorders such as arthritis (inflammation of the joint), bursitis (inflammation of the tissues around the joint). Those who have symptoms may experience ‘First step’ pain (stone bruise sensation) after getting out of bed or sitting for a period of time. Pain after driving. Pain on the bottom of your heel. Deep aching pain. Pain can be worse when barefoot.
Diagnosis
A physical exam performed in the office along with the diagnostic studies as an x-ray. An MRI may also be required to rule out a stress fracture, or a tear of the plantar fascia. These are conditions that do not normally respond to common plantar fasciitis treatment.
Non Surgical Treatment
A number of conservative measures can help take stress off the plantar fascia and encourage healing, including Icing, Taping the arch and bottom of the foot, Stretching, especially the calf, Avoiding walking with bare feet, especially on hard surfaces, Wearing orthotics or arch supports, Taking over-the-counter anti-inflammatories. If these methods fail, we generally try one of two things, A cortisone injection can help reduce swelling. Often a single injection will do the trick, but occasionally a second injection may be needed. Alternatively, we can try extracorporeal pulse activation therapy, or EPAT. This method uses sound waves to penetrate to the plantar fascia and stimulate the body’s healing response. We typically do one treatment a week for three weeks, with complete healing taking between nine to 12 weeks.

Surgical Treatment
When more conservative methods have failed to reduce plantar fasciitis pain, your doctor may suggest extracorporeal shock wave therapy, which is used to treat chronic plantar fasciitis. Extracorporeal shock wave therapy uses sound waves to stimulate healing, but may cause bruises, numbness, tingling, swelling, and pain. When all else fails, surgery may be recommended to detach the plantar fascia from the heel bone. Few people need surgery to treat the condition.
Stretching Exercises
Calf stretch. Lean forward against a wall with one knee straight and the heel on the ground. Place the other leg in front, with the knee bent. To stretch the calf muscles and the heel cord, push your hips toward the wall in a controlled fashion. Hold the position for 10 seconds and relax. Repeat this exercise 20 times for each foot. A strong pull in the calf should be felt during the stretch. Plantar fascia stretch. This stretch is performed in the seated position. Cross your affected foot over the knee of your other leg. Grasp the toes of your painful foot and slowly pull them toward you in a controlled fashion. If it is difficult to reach your foot, wrap a towel around your big toe to help pull your toes toward you. Place your other hand along the plantar fascia. The fascia should feel like a tight band along the bottom of your foot when stretched. Hold the stretch for 10 seconds. Repeat it 20 times for each foot. This exercise is best done in the morning before standing or walking.
What Leads To Heel Discomfort And Ways To Eliminate It
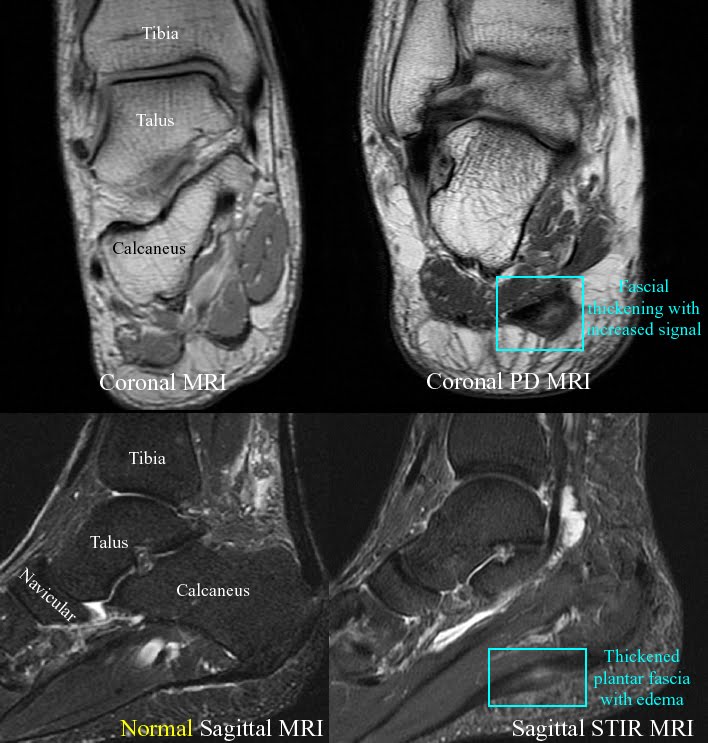
Overview
Heel pain is a common foot condition. It's usually felt as an intense pain when using the affected heel. Heel pain usually builds up gradually and gets worse over time. The pain is often severe and occurs when you place weight on the heel. In most cases, only one heel is affected, although estimates suggest that around a third of people have pain in both heels. The pain is usually worse first thing in the morning, or when you first take a step after a period of inactivity. Walking usually improves the pain, but it often gets worse again after walking or standing for a long time. Some people may limp or develop an abnormal walking style as they try to avoid placing weight on the affected heel.
Causes
Identified risk factors for plantar fasciitis include excessive running, standing on hard surfaces for prolonged periods of time, high arches of the feet, the presence of a leg length inequality, and flat feet. The tendency of flat feet to excessively roll inward during walking or running makes them more susceptible to plantar fasciitis. Obesity is seen in 70% of individuals who present with plantar fasciitis and is an independent risk factor. Studies have suggested a strong association exists between an increased body mass index and the development of plantar fasciitis. Achilles tendon tightness and inappropriate footwear have also been identified as significant risk factors.
Symptoms
If you have Plantar Fasciitis, you will most likely feel a sharp pain under the ball of you heel and it will often give pain when standing after a period of rest. For example when you get out of bed in the mornings or after being sat down. Some patients describe this feeling as a stone bruise sensation, or a pebble in the shoe and at times the pain can be excruciating. Patients with Plantar Fasciitis can experience pain free periods whereby the think they are on the mend, only for the heel pain to come back aggressively when they appear to have done nothing wrong. If your plantar fasciitis came on very suddenly and the pain is relentless, then you may have Plantar Fascial Tears. We will be able to differentiate between these 2 conditions, sometimes with ultra sound imaging. The treatment for each of these conditions will need to be very different.
Diagnosis
Your doctor will check your feet and watch you stand and walk. He or she will also ask questions about your past health, including what illnesses or injuries you have had. Your symptoms, such as where the pain is and what time of day your foot hurts most. How active you are and what types of physical activity you do. Your doctor may take an X-ray of your foot if he or she suspects a problem with the bones of your foot, such as a stress fracture.
Non Surgical Treatment
Sometimes physical therapy modalities are helpful. The most frequently used modalities include ultrasound (high frequency sound vibrations that create a deep heat and reduce inflammation) and galvanic electrical stimulation ( a carefully applied intermittent muscular stimulation to the heel and calf that helps reduce pain and relax muscle spasm, which is a contributing factor to the pain). This treatment has been found most effective when given twice a week. Repeated taping and padding is sometimes used. The felt pads that will be strapped to your feet will compress after a few days and must be reapplied. While wearing them they should be kept dry, but may be removed the night before your next appointment. Resistant cases of heel pain caused by plantar fasciitis, heel spurs or cases of stress fracture of the calcaneus often need to be placed in a removable below knee cast boot. It is important to be aware of how your foot feels over this time period. If your foot is still uncomfortable without the strapping, but was more comfortable while wearing it, that is an indication that the treatment should help. Remember, what took many months or years to develop can not be eliminated in just a few days.

Surgical Treatment
In cases that do not respond to any conservative treatment, surgical release of the plantar fascia may be considered. Plantar fasciotomy may be performed using open, endoscopic or radiofrequency lesioning techniques. Overall, the success rate of surgical release is 70 to 90 percent in patients with plantar fasciitis. Potential risk factors include flattening of the longitudinal arch and heel hypoesthesia as well as the potential complications associated with rupture of the plantar fascia and complications related to anesthesia.
What Is Heel Pain And Find Out How To Deal With It

Overview
The plantar fascia is a thick band of connective tissue that runs along the underneath of the foot from the heel bone to the toes. At the heel it can also have fascial connections to the achilles tendon. Its job is to maintain the arch of the foot, it acts as a bowstring pulled between the heel and the toes. "Itis" as a suffix indicates inflammation, but with the plantar fascia there is still some controversy over what exactly happens to the tissue when it becomes painful.
Causes
The most common cause of plantar fasciitis relates to faulty structure of the foot. For example, people who have problems with their arches, either overly flat feet or high-arched feet, are more prone to developing plantar fasciitis. Wearing non-supportive footwear on hard, flat surfaces puts abnormal strain on the plantar fascia and can also lead to plantar fasciitis. This is particularly evident when one’s job requires long hours on the feet. Obesity may also contribute to plantar fasciitis.
Symptoms
Patients with plantar fasciitis typically experience pain underneath the heel and along the inner sole of the foot. In less severe cases, patients may only experience an ache or stiffness in the plantar fascia or heel that increases with rest (typically at night or first thing in the morning) following activities which place stress on the plantar fascia. These activities typically include standing, walking or running excessively (especially up hills, on uneven surfaces or in poor footwear such as thongs), jumping, hopping and general weight bearing activity. The pain associated with this condition may also warm up with activity in the initial stages of injury. As the condition progresses, patients may experience symptoms that increase during sport or activity, affecting performance. In severe cases, patients may walk with a limp or be unable to weight bear on the affected leg. Patients with this condition may also experience swelling, tenderness on firmly touching the plantar fascia (often on a specific spot on the inner aspect of the heel) and sometimes pain on performing a plantar fascia stretch.
Diagnosis
Your doctor will check your feet and watch you stand and walk. He or she will also ask questions about your past health, including what illnesses or injuries you have had. Your symptoms, such as where the pain is and what time of day your foot hurts most. How active you are and what types of physical activity you do. Your doctor may take an X-ray of your foot if he or she suspects a problem with the bones of your foot, such as a stress fracture.
Non Surgical Treatment
Many types of treatment have been used to combat plantar fasciitis, including injections, anti-inflammatory medications, orthotics, taping, manipulation, night splinting, and instrument-assisted soft-tissue manipulation (IASTM). IASTM begins with heat, followed by stretching. Stretching may be enhanced by applying ice to the plantar fascia. These stretches should be performed several times per day, with the calf in the stretched position. IASTM uses stainless-steel instruments to effectively access small areas of the foot. IASTM is believed to cause a secondary trauma to injured soft tissues as part of the healing process. Therapeutic modalities such as low-level laser, ultrasound, and electrical muscular stimulation may be effective in the reduction of pain and inflammation. Low Dye strapping or taping of the foot is an essential part of successful treatment of plantar fasciitis. Extracorporeal shock-wave therapy (ESWT) was introduced with great promise at one time. Recent studies have reported less favorable results. Some report no effect. Previous local steroid injection may actually have a negative effect on results from ESWT.
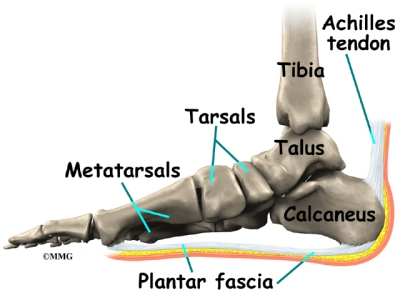
Surgical Treatment
Most patients have good results from surgery. However, because surgery can result in chronic pain and dissatisfaction, it is recommended only after all nonsurgical measures have been exhausted. The most common complications of release surgery include incomplete relief of pain and nerve damage.
Stretching Exercises
Stretching your plantar fasciitis is something you can do at home to relieve pain and speed healing. Ice massage performed three to four times per day in 15 to 20 minute intervals is also something you can do to reduce inflammation and pain. Placing arch supports in your shoes absorbs shock and takes pressure off the plantar fascia.
Ball Of Foot Pain (Metatarsalgia)
One of the hardest things to detect is the foot pain bone that is causing a severe foot pain on top of the foot of many women. Our feet are the most used (and abused) part of our body. Are you one of those people who are said to be flat footed? As humans are bipeds, they depend on their feet all day long. Foot pain should not be a part of your daily life.
Well, Mimi, we still have the same effective Walkfit design as before but we've added two significant changes. We added a specialized gel pad where it counts most, directly under the heel. I'd get a pair of Walkfits just to keep my feet fresh and I'd give a pair to everyone I know. It supports both sides and the back of your foot to help lock the foot in and keep the heel from rolling. And most important, the Walkfit flexes to help absorb shock and then returns the energy to your foot to help you walk. Your foot actually conforms to the Walkfit, not the other way around. It's like those back chairs that place your back and spine in the correct position to alleviate the pressure and the pain, and the Walkfit does the same for your feet. Along with the new gel pad, we now have an orthotic that protects, stabilizes, cushions and absorbs shock like nothing else. If I don't wear 'em, then my feet ache again.
Athletes foot is a common skin condition causing itchy, flaky skin and a burning sensation usually between the toes. Flat feet are usually the result of one's own genetics inherited from their family. Flattening is a normal part of the walking cycle of the foot, and in fact this is how the body disperses much of the shock forces created with walking. However, in some individuals, the foot flattens outward too much. This changes the way certain muscles in the foot and leg have to function, which causes numerous changes to the feet over time. These changes can include chronic straining of ligaments and tendons, as well as the development of deformities that rely on structural imbalance like bunions and hammertoes. There are numerous ways to treat flat feet.
A podiatrist, is a foot specialist, and goes to school for a lot of years to be able to hold someone's foot in their hands and listen to the type of pain you're suffering from and be able to tell you what the problem is. You should expect your doctor to ask you about the types of shoes you wear and what physical activity you engage in that might have resulted in the foot pain. The x-ray can tell the doctor if there are small breaks, fractures or fissures that could be causing your foot pain. MRI machines (magnetic resonance imaging) can be used in the same way as the x-ray to see inside your foot without having to cut you open. The doctor can then tell if there are any problems with the bones and the soft tissue inside the foot. Mild to Severe Pain: Human foot has 30 joints and 28 bones.
Top cooked fish and plantain with rest of the citrus marinade.  The plantain won't have a strong taste. I'll see if these offer any additional protection for my next long run.   Metatarsals are the long bones in your foot. Actually prevents over-movement of metatarsals so the ball of your foot is pain-free. The Associated Press gives a short rundown on the top toner shoes by brand here.
Participants were asked to indicate when the sensation of pressure changed to onset of pain. The paper grip test was used as a clinical measure of hallux plantarflexion strength 38 , 39 Participants completed three trials of three seconds, and a pass was recorded if the individual could hold the paper under the hallux against resistance for all trials.

Light and washable, they also have specially designed air vents to help keep your feet cool. We'll also include this bottle of soothing peppermint lotion to invigorate your feet and your spirit... And our special sandal adapters, so you'll never be without your Walkfits. It inhibits and kills fungus and bacteria, so no more stinky, sticky feet. And don't forget, we have holes in the Walkfit to keep your feet cool all the time.
Can Working On Your Computer Cause
There are different types of foot fungus that occur due to many factors both internally and externally, that can alter one's physical state, foot wise. Every day there are many women around the world that wish that they could change the way that their skin looks.

However if you use the right medication, athletes foot can be eliminated through the body system. The reaction occurs based on the body's immune system; however it's always better to exercise proper foot care if you do contract the fungus. This isn't true as shoes with good ventilation don't create moist and warm conditions or lead to athlete's foot. Take preventive care by wearing cotton socks, washing socks everyday and drying the feet after washing or bathing. Now that all these myths have been clarified, just follow a strict and regular hygiene regimen to prevent athlete's foot. Self treatment may lead to more significant problem.
Long hours of work under conditions of stress put an extra burden on the feet. When your feet get painful you concentrate on them instead of the work. When feet become strained and painful they should be studied by an orthopedic surgeon. Don't ignore pain: Painful feet are not normal.

Hands at times also get infected with calluses, but the use of pumice stone is not advised for removal of calluses on hands. The process is a bit slow, but the treatment is permanent and guaranteed without any side effect. There are surgical treatments as well where your doctor will cut the hard skin but only few people resort to this option. As far as medication is concerned salicylic acid ointments is often used to remove the hard portions of the skin. Complications caused by calluses should be consulted with podiatrist as it can also cause infection in certain number of ways. The treatment of callus depends upon its nature and severity. But some of the treatments out there are very hard and damaging to your skin.
It is a condition where brownish raised skin bumps appear around the areas of the armpits, groin, on the side of one's neck, knees, elbows and hands. Diabetes can be a possible reason for any of the above mentioned symptoms or it might be possible that the patient is allergic to diabetic medication too. It is very important that we understand the fundamental differences of various salon to get the most out of them.
Foot Problems Are Genetic
A bunionette is similar to a bunion, but it develops on the outside of the foot. Kate Middleton is barely seen out in public engagements without her trusty nude LK Bennett high heels on. When she made a pre-Olympic visit to a judo center however, she gamely kicked off her heels to step on the mat. Pain is a symptom common to many foot conditions, and pain medications are a good solution for most types of foot pain.
Elderly people wearing shoes with thick inflexible soles may be unable to sense the position of their feet relative to the ground, significantly increasing the risk for falling. If shoes need breaking in, place moleskin pads next to areas on the skin where friction is likely to occur.
Below is a series of questions that podiatrists commonly ask in order to find the source of the pain and how to better treat it. Patients should think about some of the answers to the following questions before and during the appointment in order to better assist the podiatrist in finding the source of the problem. Aside from treating the source of the problem, the podiatrist may offer treatment that can alleviate pain. Josie, now 2 years old, still has some health conditions and has had several close calls in her young life.
Most cases of foot pain can be treated without surgery, whether it's metatarsal foot pain, ball-of-foot pain, foot arch pain or some other type. At the start to notice soreness or discomforts around the foot area, it is imperative to take rest, put on or apply cold or ice compress, and or elevate the affected foot. Generally, foot pains vary from mild to severe. However, prevention is above all better than to deal with any pain though. Never take for granted to any pain; focus on getting foot pain reliever at the soonest is vital. In case the pain is unbearable which it hampers the usual life activities, it is imperative to look for urgent medical or therapist to help and also consider the ordinary methods to lessen foot pain. Stretching exercises also facilitate to soothe the muscles on the feet and help out in the contraction of the muscles. Not all skin disorders respond to treatment.
A lot of professionals believe that common physical activity may be the answer to gout. You'll want to have an expert to look at the concerns with your feet. The feet might be experiencing pain for a lot of numerous reasons. The deep tissue massage is ideal for people experiencing chronic muscle pain on their upper and lower back, legs, and shoulders. A deep tissue massage frees our muscles of toxin build-up that is usually the main cause of pain and muscle immobility. Some massage therapists call it pressure therapy" since it involves applying pressure to specific points on the foot. A foot massage is a very relaxing way of addressing problems with your body's internal organs. A trained massage therapist can also put pressure on different meridians or energy lines on the sole and side of the feet to determine the cause of illness. A sports massage is ideal of active individuals that are engaged in sports or intensive work-outs. However, they may be contagious for weeks after symptoms go away.
Even when you are experiencing ankle, knee, leg or back pain podiatry Windsor can often help. Podiatry Windsor is really no different than a dentist; we should all get regular checkups, even when nothing seems wrong, to ensure we take care of the health of our feet. However some of the important reasons to get a consultation with a Podiatrist are; persistent foot or ankle pain that won't go away with rest, ice or anti-inflammatories, a wound or sore that does not heal, foot discolorations (if one foot is a much different color than the other), any pain or swelling, and numbness, burning or tingling in the feet. An important thing to point out is that podiatry Windsor is a very good preventative practice. Below is Dr Foot's 20 foot care tips.
To stop foot pain it is advisable to wear shoes that are well cushioned and have a flexible area at the ball of the foot. For severe conditions doctors and podiatrists may recommend orthotics or orthoses. These are insoles which are specifically modelled from plaster cast of the patient's foot. Orthopaedic footwear is also good in treating foot pain. For correct treatment of widespread orthopedic issues within the foot it is required to make use of orthopedic sneakers regularly. The feminine part of the sufferers are more likely to immediately hurry to buy only essentially the most beautiful models of orthopedic sneakers for women Nonetheless, do consult your orthopaedist prior to purchase, as he will recommend probably the most suitable footwear needed to your specific feet situation. Bunions can also be a result of arthritis, which often affects the big toe joint. There are numerous ways to treat flat feet.

Metatarsal Pain
See how much softer and smoother my skin looks in the second photo? Corns and calluses can be painful and frustrating problems in the foot. The stretching foot rocker is a helpful tool in relieving pain associated with lower leg conditions. Alton Beauty has now added Callus Peel to the range of pedicure treatments. Everybody, from school children on can recognize a wart.
The boring bits, like the kneecaps, unless you have a fetish for kneecaps, the sometimes unpleasant parts, like the callous on your foot serving as a hat to your bunion, the parts you just wonder about, like your weenus, and yes, the beautiful aspects, perhaps the eyes, the smile, or the hands. My friend Sergio gave it to me, and he told me that he has had it for 7 or 8 years, and its really special to him. Simply apply the Softener Gel to a Foot Patch. After just a few minutes, use the Scraper to peel and scrap away those ugly calluses. Next for the finishing touch use the file to smooth out the skin and apply the Foot Balm to achieve baby soft supple feet! A manicure involves trimming fingernails, removing excess cuticle, and adding nail polish (with color or just a clear top coat). A pedicure is the same thing for your feet. When you get a facial you get more of a spa experience than just a pedicure or manicure.
Sometimes, the pressure of the corn or callus may cause inflammation, which can result in pain, swelling and redness. The body protects skin tissues from pressure or friction damage by producing an area of hard skin. So unless the cause of the pressure or friction is found and removed, calluses and corns will continue to form. Over-the-counter treatments, such as corn plasters, can damage the healthy surrounding skin if you use them incorrectly. Look at and feel each foot for signs of injury including bruises, blisters, broken or cracked skin, hot or cold areas, corns and calluses, and discolouration. If your eyesight is poor, get someone else to check your feet for you. Tinea is a contagious fungal infection of the skin. It usually develops between the toes and along the arch of the foot.
A clavus is a thickening of the skin due to intermittent pressure and frictional forces. The word clavus has many synonyms and innumerable vernacular terms, some of which are listed in the Table below; these terms describe the related activities that have induced clavus formation. The shape of the hands and feet are important in clavus formation. Specifically, the bony prominences of the metacarpophalangeal and metatarsophalangeal joints often are shaped in such a way as to induce overlying skin friction. Toe deformity, including contractures and claw, hammer, and mallet-shaped toes, may contribute to pathogenesis. First, you had better prepare for a basin of warm water to soak the feet every winter night.

Well, corns (Heloma) are small and round: they also have a hard thickening bit of skin in the middle and are very painful. They usually affect your smaller toes; and wearing poorly fitted shoes can cause excessive friction and rubbing of the skin to form a corn. When people opt to use products containing Aloe Vera, such as gels and creams, they can prevent and remove corns. Common foot problems and nail deformities in our aging population.
